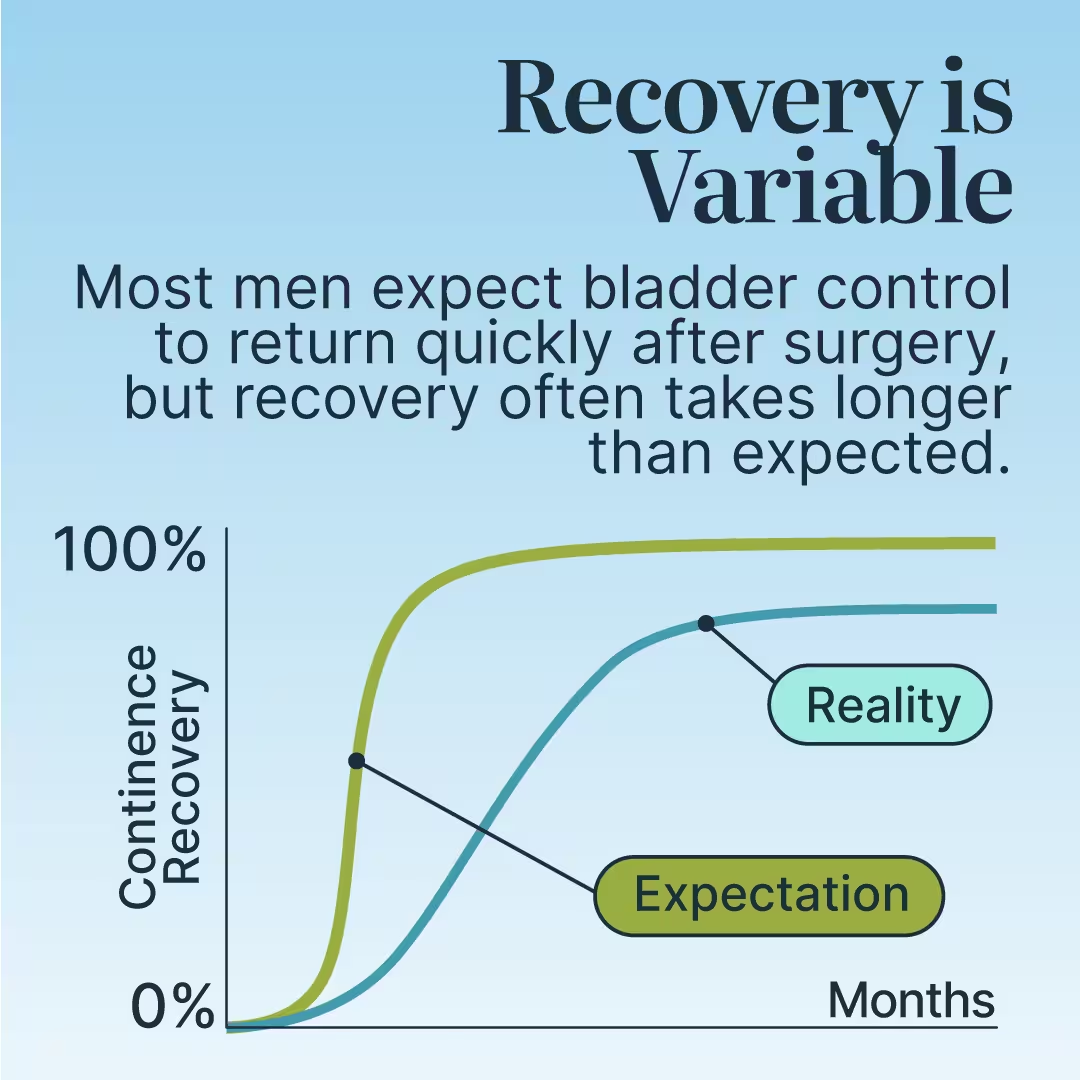
Regaining continence after prostatectomy depends on the pelvic floor muscles and the external urethral sphincter taking over a greater role in urinary control. While most men gradually recover, the process can be slower or more difficult for some patients due to several physiological and behavioral factors.
Post-surgical neuromuscular changes
Prostate surgery can temporarily affect the nerves and muscle coordination involved in continence. Even when a patient attempts to contract the pelvic floor correctly, muscle activation may initially be weak or inconsistent as the neuromuscular system recovers.
Difficulty performing effective pelvic floor contractions
Many men are unfamiliar with the pelvic floor muscles and may struggle to identify or isolate them correctly. It is common for patients to substitute with abdominal, gluteal, or thigh muscles, limiting the effectiveness of pelvic floor training.
Inconsistent adherence to rehabilitation exercises
Pelvic floor strengthening typically requires regular training over weeks to months. Without feedback or structured programs, adherence can decline, reducing the likelihood of meaningful strength and coordination improvements.
Individual variation in healing and recovery
Age, baseline muscle condition, nerve preservation during surgery, and surgical technique all influence recovery timelines. As a result, continence recovery varies widely between patients, and some men require additional support to restore pelvic floor function.
Sources:
American Urological Association. Incontinence after Prostate Treatment Guideline.
Ficarra V. et al., European Urology, 2014. Systematic review of continence outcomes after radical prostatectomy.